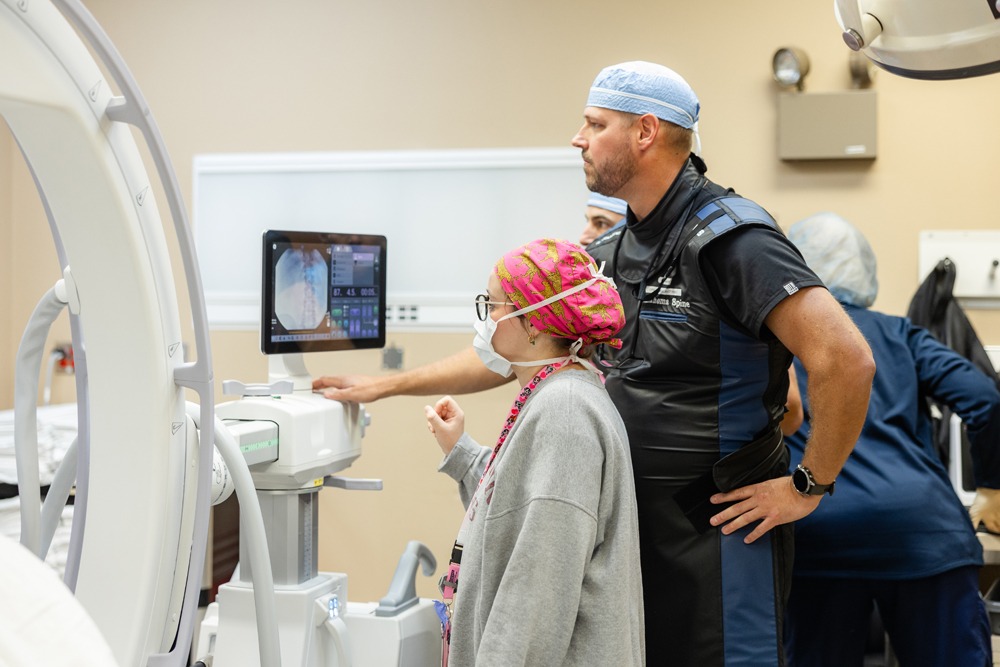
Kyphoplasty is a minimally invasive procedure to relieve pain due to vertebral compression fracture. The procedure is typically performed under general or local anesthesia. You will lie face down on the operating table. Using live X-ray imaging, your doctor will insert a large needle through the skin into the vertebra and insert a balloon through the needle. The balloon is then inflated to help restore some of the vertebra’s height and reduce spinal deformity. The balloon is then removed and the empty space created between the vertebrae is injected with cement. The cement quickly hardens restoring height and providing strength and stability to the vertebra.
What are the Indications?
Kyphoplasty is indicated for painful vertebral compression fractures (VCFs) from osteoporosis, trauma, or cancer (like multiple myeloma, metastases) that cause severe, intractable back pain not relieved by conservative treatments (meds, PT, bracing). It’s for acute/chronic fractures with severe pain, height loss, or progressive deformity (kyphosis) and aims to stabilize the vertebra, restore height, and reduce pain, especially in older adults with weakened bones
Preparing for a kyphoplasty
Prior to the procedure, you will meet with your doctor to go over all the risks and benefits of the Kyphoplasty. As it is a medical procedure, your doctor may order blood tests. The doctor may also order an MRI and x-rays to help the doctor determine the precise area of your vertebrae that needs attention. Once you fully understand the procedure, and we’ve explained all risks and ordered all tests, we will schedule your kyphoplasty.
You should not eat or drink anything 8 hours before the surgery. You may take your medications with a sip of water unless otherwise directed by the Anesthesiology team. You may have to temporarily discontinue certain medications such as blood thinners or diabetic medication. The procedure may not be performed if you have an ongoing infection, elevated blood glucose or elevated blood pressure.
What to expect during your procedure?
You will check into the facility at your scheduled time. You will be asked to fast for 8 hours prior to your procedure. You will be brought back and prepped by a nurse on staff. They will insert the IV to be used for your anesthesia. You will meet with the anesthesiologist and your doctor prior to the procedure. Once you’re taken to the procedure room you will be put under general anesthesia and placed in the prone position and a fluoroscopy machine will be brought into position. Your doctor will then numb the area with a local anesthetic and using live fluoroscopic guidance to perform the procedure. The whole procedure takes less than one hour for the majority of cases.
What to expect after the procedure?
After your procedure, we will take into a recovery room; we will remove your IV, and a nurse will closely monitor you while you wake up from your anesthesia and administer medicine for pain control or to treat nausea as needed. You will be asked not to drive for at least 24 hours after the procedure, and you must have a driver to drive you home from the hospital once you’re discharged. You may feel some discomfort in the injection areas that could last a few days, but can resume normal activity almost immediately. Pain relief for many may be immediate. However, for some, it may take days to feel the full effects of the procedure. You will be seen in office for follow up approximately 10 days after the procedure. Heavy lifting and any strenuous activities should also be avoided for at least 6 weeks after the surgery.
What risks or complications are associated with the procedure?
As with any procedure, a kyphoplasty may be associated with certain risks and complications such as pain (temporary), bruising, infection, bleeding, reaction to anesthesia, and leakage of bone cement to surrounding areas. Serious complications are uncommon and afterward you should experience considerable relief from pain and improved quality of life.
Is there anything my doctor needs to know prior to the procedure?
You should tell your doctor if you are pregnant, on blood thinners, diabetic, or if you have any other concerns you would like to address beforehand.
The above information is for general education purposes only. Please ask your doctor any specific questions you may have during your visit.

